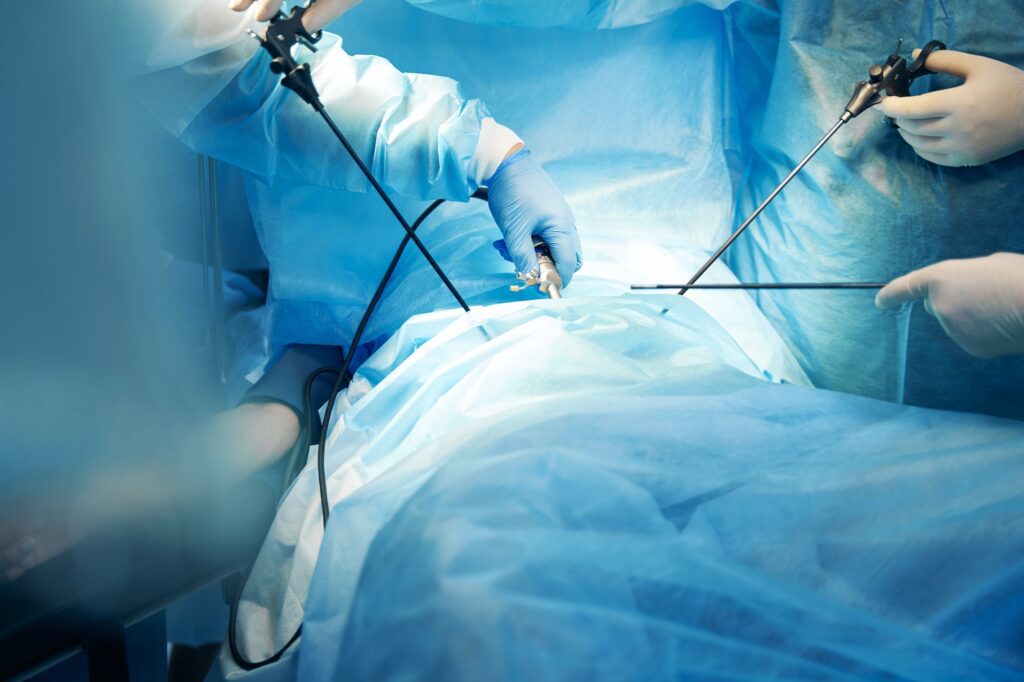
Laparoscopic surgery is a minimally invasive surgery in which the abdomen is inflated with air and then the surgery is performed through several ½ -1 inch incisions using small telescopes and small instruments. The incisions are placed around the organ being operated on. Usually a small incision is made to remove the organ if it is diseased or cancerous. Repair or removal of the kidney, adrenal, prostate and other urologic organs or cancers are possible laparoscopically and have become the standard of care in many cases.
What are the benefits of Laparoscopic Surgery (laparoscopy)?
The benefits usually are: reduced trauma to the body, less anesthesia, often less blood loss and need for transfusions, less postoperative pain and discomfort, less risk of infection, shorter hospital stay, faster recovery and return to normal daily activities, and less scarring and improved cosmesis.
What are the risks of laparoscopy?
There are the usual risks when you have general anesthesia that involves your heart, brain and lungs. The abdominal organs, glands, intestines, or blood vessels may be damaged. The doctor may need to perform open abdominal surgery to repair them at the time of the procedure or post operatively. You may develop an infection or bleeding. A blood clot may break off, enter the bloodstream, and clog an artery in your lungs, abdomen, pelvis, heart or brain or legs. These same risks are also possible in open surgical procedures. These complications are rare but can occur.
How do I prepare for laparoscopy?
Plan for your care and recovery after the operation. Allow for time to rest and try to find other people to help you with your day-to-day duties. Follow instructions provided by your doctor. You may need to drink something to clear your bowels the day before surgery. Do not eat or drink anything after midnight and the morning before the procedure. Do not even drink coffee, tea, or water and only take your medicines that you are told to take with a sip of water. Stop all aspirin, motrin, coumadin and other blood thinner medications beforehand as instructed.
What happens during the procedure?
A general anesthetic is given, which relaxes your muscles, makes you feel as if you are in a deep sleep, and prevents you from feeling pain. Your peritoneal cavity is inflated with carbon dioxide gas. This expands your peritoneal cavity like a balloon and helps the doctor see your organs. The doctor makes a small cut near your bellybutton, puts in the gas, puts a laparoscope into the abdominal cavity, and puts another tool through a small cut in the abdomen. The doctor guides the scope to look at your abnormal organ. He then exposes the area and repairs or removes the abnormal organ. The abnormal organ or tumor is sent to the laboratory for analysis.
What happens after the procedure?
You may stay in the hospital for a few hours or overnight for several days to recover. The anesthetic may cause sleepiness or grogginess for a while. You may have some shoulder pain, feel bloated, or find a change in bowel habits for a few days. You may not be able to urinate right away and may have a catheter (a small tube) placed into your bladder through the urethra (the tube from the bladder to the outside) for a few days. You should avoid heavy activity such as lifting. You should ask your doctor how much you should lift, what other steps you should take, and when you should come back for a checkup.
When should I call the doctor in the postoperative period?
Call the doctor if: You develop excessive redness, swelling, pain, or drainage from the small incisions. You become dizzy and faint or have fevers over 101. You develop uncontrolled nausea and vomiting. You become constantly short of breath. You develop abdominal pain or swelling that gets worse or you are unable to have a bowel movement after 3 days. Call the office or the doctor on questions or problems before or after your operation.